PCOS Natural Management — Diet, Supplements, and Lifestyle
Evidence-based strategies for managing PCOS naturally through diet modifications, targeted supplements like inositol and omega-3s, exercise, and stress management.
13 Min Read
The short version: PCOS affects 5-15% of reproductive-age women and there is no cure, but diet modifications, targeted supplements like inositol and omega-3s, regular exercise, and stress management can reduce symptoms and improve metabolic markers. Lifestyle changes are recommended as the first-line intervention by international PCOS guidelines.
What PCOS Actually Does to Your Body
Polycystic ovary syndrome is the most common endocrine disorder in women of reproductive age, affecting somewhere between 5% and 18% of women depending on which diagnostic criteria you use. The name is misleading, though. You don't need ovarian cysts to have PCOS, and the condition goes well beyond your ovaries.
PCOS is a metabolic and hormonal disorder. Your ovaries produce abnormally high levels of androgens (male hormones that all women produce in smaller amounts), and that throws off the normal ovulation cycle. According to the Cleveland Clinic, a diagnosis typically requires at least two of three features: irregular or missed periods, signs of excess androgens (acne, excess hair growth, or elevated blood levels), and polycystic-appearing ovaries on ultrasound.
But what drives much of the damage is happening below the surface. Insulin resistance is the engine here. When your cells stop responding efficiently to insulin, your body pumps out more of it. That extra insulin tells your ovaries to produce even more androgens, which worsens everything. The Mayo Clinic points to insulin resistance, low-grade chronic inflammation, genetics, and excess androgen production as the primary factors.
The effects don't stop at irregular periods. Women with PCOS face higher risks of type 2 diabetes, cardiovascular disease, nonalcoholic fatty liver disease, depression, anxiety, sleep apnea, and endometrial cancer. Between 40% and 80% of women with PCOS have obesity, which makes insulin resistance and inflammation worse.
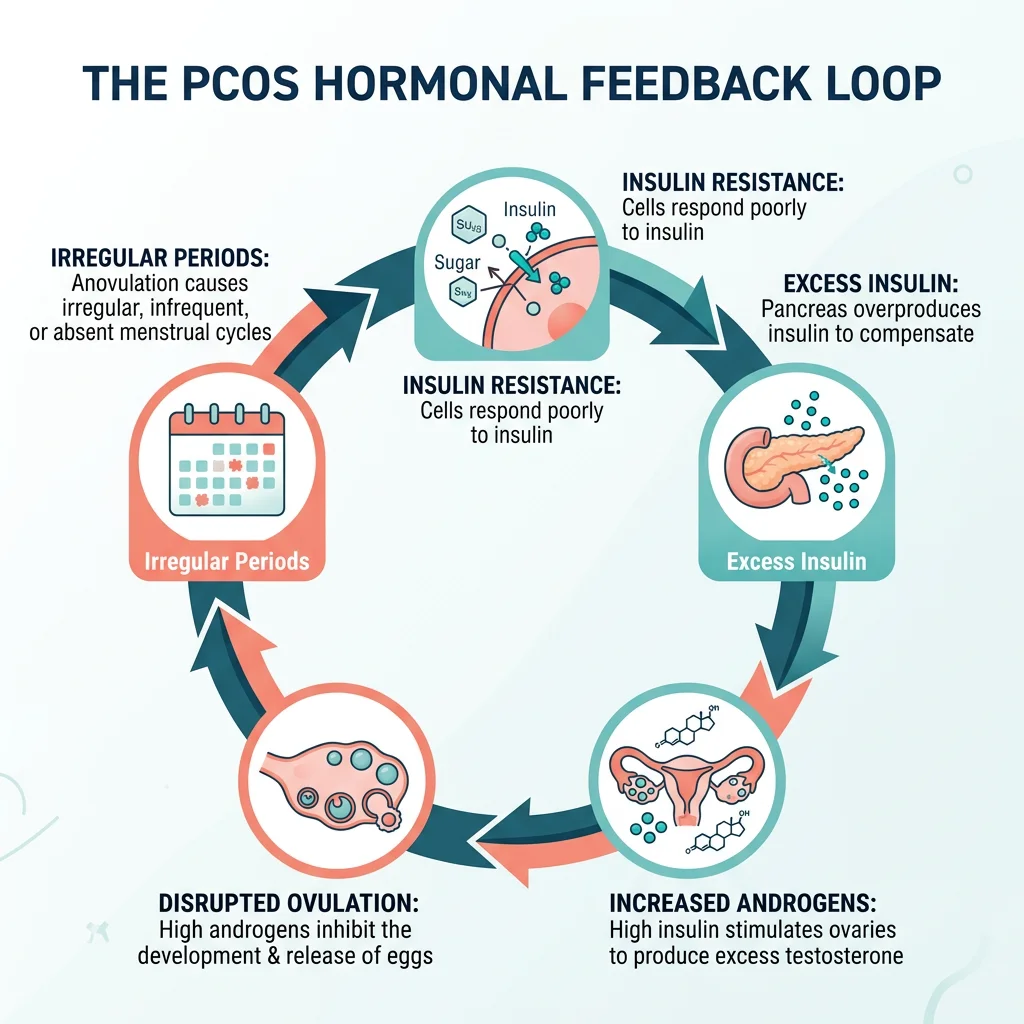
This matters for one reason: it explains why lifestyle interventions work. If insulin resistance is what kicks off the hormonal cascade, then anything that improves insulin sensitivity -- a specific way of eating, certain supplements, exercise -- can interrupt that cycle and dial down symptoms. The 2025 international evidence-based guidelines now put lifestyle modifications ahead of pharmaceutical intervention as the primary early strategy for PCOS management.
Diet Changes That Actually Help
There is no single "PCOS diet," but the research keeps pointing in the same direction: eat in ways that improve insulin sensitivity and tamp down inflammation. A 2022 review in the Journal of Food Biochemistry recommended a macronutrient split of roughly 40% carbohydrates, 30% fats, and 30% protein as a starting framework for women with PCOS, paired with regular physical activity.
Low-glycemic foods over refined carbohydrates
The glycemic index (GI) measures how quickly a food raises blood sugar. Low-GI foods -- whole grains, legumes, most vegetables, some fruits -- produce a slower, steadier glucose response. High-GI foods like white bread, sugary drinks, and processed snacks spike your blood sugar fast, which triggers more insulin release. That's the opposite of what an insulin-resistant system needs.
A 2024 review in PMC found that Mediterranean-style dietary patterns with a focus on high fiber and low-GI carbohydrates may be especially helpful for targeting insulin resistance in women with overweight or obesity and PCOS.
The Mediterranean pattern
The Mediterranean diet hits most of the right notes for PCOS. Lots of vegetables, fruits, whole grains, legumes, nuts, olive oil, and fish. Less red meat, processed food, and added sugar. It's naturally anti-inflammatory, high in fiber, and moderate in healthy fats. A 2025 systematic review in Nutrients found these properties improve both insulin sensitivity and hormonal balance in women with PCOS.
| Food Category | Include More | Limit or Avoid |
|---|---|---|
| Carbohydrates | Quinoa, oats, sweet potatoes, legumes | White bread, pastries, sugary cereals |
| Proteins | Fatty fish, chicken, eggs, tofu, lentils | Processed meats, fried proteins |
| Fats | Olive oil, avocado, nuts, seeds | Trans fats, excessive saturated fat |
| Dairy | Greek yogurt, fermented options | Full-fat dairy in excess (may worsen acne) |
| Beverages | Water, green tea, herbal teas | Soda, fruit juices, energy drinks |
Anti-inflammatory foods
Chronic low-grade inflammation is a hallmark of PCOS. The Nutrients systematic review confirmed that antioxidant-rich and anti-inflammatory diets improve both insulin sensitivity and hormonal balance. In practice, that means berries, leafy greens, fatty fish (salmon, sardines, mackerel), turmeric, ginger, and extra virgin olive oil. If you want to go deeper on anti-inflammatory eating, our guide to evidence-based nutrition covers the research behind specific food choices.
What about calorie restriction?
Losing just 5% of body weight can improve hyperandrogenism, insulin resistance, fertility, and menstrual function in women with PCOS who carry extra weight, according to the 2024 Frontiers in Endocrinology review. But crash diets and severe restriction tend to backfire -- they jack up cortisol and make hormonal imbalance worse. A moderate caloric deficit of 500-750 calories per day, combined with better food quality, tends to work better and last longer than drastic cuts.
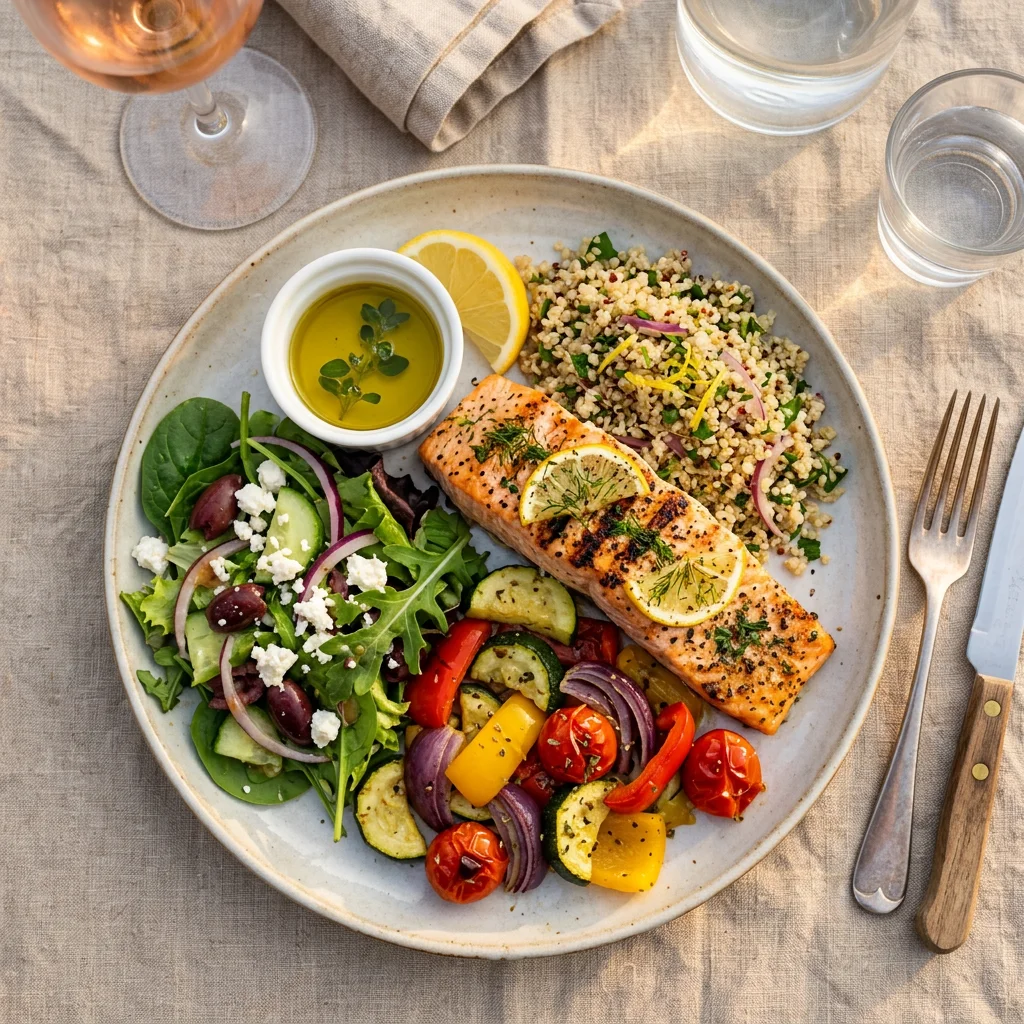
Supplements Worth Considering
Supplements won't replace good eating habits and regular movement, but a few of them have enough clinical evidence behind them to be worth talking to your doctor about. A 2025 umbrella meta-analysis that pulled together 46 randomized trials with over 30,000 participants found that inositol, probiotics, and omega-3 fatty acids showed the most consistent benefits across multiple PCOS outcomes.
Inositol (myo-inositol and D-chiro-inositol)
Inositol is the supplement that gets the most attention in PCOS research, and for good reason. Myo-inositol and D-chiro-inositol act as secondary messengers for insulin, and when the ratio between them gets off, it contributes to insulin resistance. A systematic review and meta-analysis in the Journal of Clinical Endocrinology & Metabolism (2024), done to inform the 2023 international PCOS guidelines, found that inositol shows benefits for some metabolic measures and potential benefits for ovulation. The umbrella meta-analysis found myo-inositol significantly improved insulin sensitivity (HOMA-IR) and sex hormone-binding globulin (SHBG) levels.
The dosing protocol used in most studies is 4,000 mg of myo-inositol combined with 100 mg of D-chiro-inositol daily, maintaining the physiological 40:1 ratio. Myo-inositol also tends to cause fewer gastrointestinal side effects than metformin, according to the same meta-analysis.
The catch: the 2024 meta-analysis for the international guidelines concluded that the evidence, while promising, is still "limited and inconclusive" for some outcomes. Inositol isn't a standard-of-care recommendation yet, but it's a reasonable option to bring up with your doctor.
Omega-3 fatty acids
Omega-3s (EPA and DHA from fish oil) go after the inflammatory and lipid problems that come with PCOS. The 2025 umbrella meta-analysis found omega-3 supplementation significantly reduced LDL cholesterol and increased HDL cholesterol in women with PCOS. The 2024 review in Frontiers in Endocrinology also noted that omega-3 PUFAs improve HOMA-IR, insulin levels, total cholesterol, and triglycerides. Study doses range from 1,000 to 3,000 mg of combined EPA and DHA daily. For more on omega-3 research, see our article on evidence-based nutrition.
Vitamin D
Vitamin D deficiency is common in women with PCOS. According to the 2024 Frontiers in Endocrinology review, vitamin D improves insulin metabolism, increases total antioxidant capacity, reduces hirsutism, and lowers C-reactive protein and testosterone levels. It also appears to regulate ovulation dysfunction through vitamin D receptor genes in the ovaries. That said, the same review notes that high doses can be toxic, and you should get your levels tested before starting supplementation.
Probiotics
The gut-health angle on PCOS caught a lot of researchers off guard. The 2025 umbrella meta-analysis found that probiotics significantly reduced systemic inflammation (measured by C-reactive protein) through gut-microbiota modulation. Women with PCOS tend to have altered gut microbiome composition, and probiotic supplementation may help rebalance things. If you're curious about the gut-hormone connection, our gut health and microbiome testing guide gets into it.
| Supplement | Primary Benefit in PCOS | Typical Study Dose | Evidence Level |
|---|---|---|---|
| Myo-Inositol | Insulin sensitivity, ovulation | 4,000 mg/day | Moderate (multiple RCTs) |
| D-Chiro-Inositol | Hormonal balance, ovulation | 100 mg/day (with MI) | Moderate |
| Omega-3 (EPA/DHA) | Inflammation, lipid profile | 1,000-3,000 mg/day | Moderate-Strong |
| Vitamin D | Insulin metabolism, androgen levels | 1,000-4,000 IU/day | Moderate |
| Probiotics | Inflammation, gut health | Strain-dependent | Emerging |
| N-Acetylcysteine (NAC) | Antioxidant, insulin sensitivity | 600-1,800 mg/day | Limited |
| Curcumin | Fasting glucose, inflammation | 500-1,500 mg/day | Limited |

Exercise and Movement Strategies
You don't need to train like an athlete to see benefits from exercise with PCOS. The 2025 systematic review in Nutrients confirmed that both aerobic exercise and resistance training improve insulin sensitivity, support weight management, and lead to better metabolic and reproductive outcomes in women with PCOS.
What type of exercise works best?
A mix of aerobic and resistance training. Aerobic exercise (walking, cycling, swimming) directly improves cardiovascular health and insulin sensitivity. Resistance training (weight lifting, bodyweight exercises, resistance bands) builds muscle mass, which raises your resting metabolic rate and creates more glucose-absorbing tissue. Both of those help fight insulin resistance.
| Exercise Type | PCOS Benefits | Recommended Frequency |
|---|---|---|
| Moderate Aerobic (brisk walking, cycling) | Insulin sensitivity, cardiovascular health, mood | 150 min/week |
| Vigorous Aerobic (running, HIIT) | Fat loss, metabolic improvements | 75 min/week |
| Resistance Training | Muscle mass, resting metabolism, glucose uptake | 2-3 sessions/week |
| Yoga | Stress reduction, hormonal regulation, flexibility | 2-3 sessions/week |
The Nutrients review also noted that yoga, mindfulness practices, and breathing exercises help by lowering cortisol levels and psychological distress, both of which tend to be elevated in women with PCOS. If you're looking for stress-reduction techniques, our guide on breathing techniques for stress relief pairs well with a PCOS management plan.
How much is enough?
International guidelines call for a minimum of 150 minutes of moderate-intensity physical activity per week, or 75 minutes of vigorous activity. For women with PCOS who carry extra weight, pairing that with a modest caloric deficit speeds things up. But even without weight loss, exercise on its own improves insulin sensitivity and lowers androgen levels. Showing up regularly matters more than going hard.
Stress, Sleep, and the Hormonal Loop
Stress management tends to get shoved to the bottom of the PCOS to-do list, but it probably shouldn't be. Cortisol (your primary stress hormone) and insulin share overlapping metabolic pathways. When stress keeps cortisol high, it promotes insulin resistance, encourages abdominal fat storage, and disrupts ovulation. Our article on how chronic stress wrecks your hormones walks through this feedback loop in detail.
Sleep matters just as much. Poor sleep quality and sleep disorders (especially sleep apnea, which the Mayo Clinic lists as a PCOS complication) make insulin resistance worse and ramp up inflammation. Getting 7-9 hours of quality sleep, keeping consistent sleep-wake times, and treating sleep disorders all help create the hormonal environment where other changes can actually take hold.
For stress management specifically, the strategies with research behind them include regular exercise (which helps your body and your head at the same time), mindfulness meditation, yoga, breathing exercises, and cognitive behavioral therapy. What works best is whatever you'll actually do consistently, not the theoretically "optimal" technique you'll abandon after a week.
PCOS Myths vs. Facts
| Myth | Fact |
|---|---|
| You need ovarian cysts to have PCOS | Despite the name, the Cleveland Clinic confirms you can have PCOS without cysts. "Polycystic" describes the follicle appearance, not actual cysts. |
| PCOS only affects overweight women | While 40-80% of women with PCOS have obesity, lean women get it too. Insulin resistance happens independently of body weight. |
| You can't get pregnant with PCOS | PCOS is the most common cause of female infertility, but most women with PCOS can conceive with treatment. Lifestyle changes alone restore ovulation in some cases. |
| Supplements can cure PCOS | No supplement cures PCOS. The 2024 review in Frontiers in Endocrinology is clear that while supplements cause metabolic changes, they "do not directly reverse the disorder." |
| Cutting all carbs is the best diet for PCOS | Carb quality matters more than cutting them out. Low-GI carbohydrates from whole grains, legumes, and vegetables improve insulin sensitivity without the downsides of going carb-free. |
| PCOS goes away after menopause | Hormonal symptoms may ease up, but metabolic risks (diabetes, cardiovascular disease) stick around for life. |
Building Your PCOS Management Plan
PCOS hits multiple systems at once, so managing it takes more than one change. A practical approach based on the current research looks something like this.
Diet quality comes first. Move toward a Mediterranean-style eating pattern with low-GI carbohydrates, lean proteins, healthy fats, and fiber. You don't have to overhaul everything at once -- swapping one processed meal per day for a whole-food option is a reasonable place to start.
Movement is next. Aim for 150 minutes of moderate activity per week. Walking plus 2-3 resistance training sessions covers it. If you're starting from nothing, try 10-minute walks after meals. Post-meal movement helps blunt blood sugar spikes.
On the supplement side, myo-inositol (with D-chiro-inositol in a 40:1 ratio), omega-3 fatty acids, and vitamin D have the most research behind them right now. Get your vitamin D levels tested before supplementing, and bring up probiotics if you also deal with gut-related symptoms. All of this should go through your doctor.
Stress and sleep aren't optional add-ons. They directly affect the hormonal pathways that drive PCOS. Pick one stress-management practice and one sleep hygiene change to start with.
For tracking, menstrual regularity is the easiest marker to watch. Other useful numbers include fasting insulin, HOMA-IR, testosterone levels, and inflammatory markers like C-reactive protein. Work with your doctor to get baseline values and re-test every 3-6 months.
And give it time. Most studies showing real improvement ran for 12-24 weeks. Three months is a reasonable minimum before evaluating whether your changes are working.

Frequently Asked Questions
Can diet alone reverse PCOS symptoms?
It can make a real dent, but probably won't fix everything on its own. A 2022 review found that a balanced diet with approximately 40% carbs, 30% fats, and 30% protein combined with physical activity could reduce severe symptoms and improve metabolic balance. How much improvement you see depends on your PCOS phenotype, body composition, and how insulin-resistant you are. Most women get the best results when they combine dietary changes with exercise and stress management.
Is inositol safe to take long-term?
Based on current evidence, it seems well tolerated. The 2024 meta-analysis in the Journal of Clinical Endocrinology & Metabolism found that myo-inositol causes fewer gastrointestinal side effects than metformin, and those side effects tend to be mild and temporary. That said, long-term safety data beyond 6-12 months is limited. Talk to your healthcare provider about ongoing supplementation, especially if you are pregnant or trying to conceive.
How quickly do lifestyle changes improve PCOS?
Most clinical trials showing meaningful improvements ran for 12 to 24 weeks. Some women notice their menstrual cycle becoming more regular within 2-3 months of consistent dietary and exercise changes. Weight loss of just 5% of body weight can improve insulin resistance, androgen levels, and ovulation in women who carry extra weight. But individual timelines vary a lot depending on where you're starting from and how consistent you are.
Do women with lean PCOS benefit from the same approach?
Yes, with some adjustments. Lean women with PCOS still benefit from anti-inflammatory eating patterns, exercise, stress management, and targeted supplements. The caloric deficit piece is less relevant and potentially harmful for women already at a healthy weight. For lean PCOS, the focus should be on food quality, insulin-sensitizing supplements like inositol, and regular movement rather than weight loss.
Should I take metformin or try natural approaches first?
International PCOS guidelines recommend lifestyle modifications as the first thing to try. Medications like metformin typically come into play when lifestyle changes alone aren't enough, or for specific situations like prediabetes. The inositol meta-analysis found it may improve similar metabolic markers with fewer GI side effects than metformin. But this is a decision you should make with your doctor based on your specific symptoms, lab values, and goals.
Related Articles
- Berberine: Nature's Metformin for Blood Sugar and Weight — Berberine shows insulin-sensitizing effects similar to metformin, making it another option worth exploring for PCOS-related insulin resistance.
- How Cortisol Drives Weight Gain and What Actually Helps — Understanding the cortisol-insulin connection explains why stress management is critical for PCOS.
- Weight Loss Supplements for Women Over 40 — Overlapping research on metabolic support supplements relevant to PCOS management.
- Rhythmic Health Revolution: Ultimate Guide to Cycle Syncing — Aligning diet and exercise with your menstrual cycle phases can complement a PCOS management strategy.
- Gut Health Personalization and Microbiome Testing Guide — The gut-hormone axis plays a growing role in PCOS research.
Medical Disclaimer
This article is for informational and educational purposes only and is not medical advice, diagnosis, or treatment. Always consult a licensed physician or qualified healthcare professional regarding any medical concerns. Never ignore professional medical advice or delay seeking care because of something you read on this site. If you think you have a medical emergency, call 911 immediately.










